Why does people with dementia get mean in the end stage:
That’s a really important—and tough—question. In the end stages of dementia, some people may seem mean or aggressive, but it’s often not intentional. These changes usually stem from the brain’s progressive damage, not from the person’s true character.
As dementia advances, especially in conditions like Alzheimer’s or frontotemporal dementia, the parts of the brain that regulate emotion, behavior, and self-control deteriorate. This can lead to:
- Frustration and fear: They may not understand what’s happening around them or recognize loved ones, which can be terrifying.
- Communication breakdown: When they can’t express needs or discomfort, it may come out as anger or agitation.
- Physical discomfort: Pain, infections, or hunger might go unnoticed or untreated, and they may lash out as a result.
- Sundowning: Many experience increased confusion and irritability in the late afternoon or evening, known as sundowning.
It’s heartbreaking, especially for caregivers who remember who the person used to be. But these behaviors are symptoms of the disease, not a reflection of the person’s feelings toward others.
If you’re caring for someone going through this, you’re not alone—and there are ways to ease the journey. Would you like tips on how to respond to these behaviors or support resources for caregivers?
Dementia is a general term for a chronic or persistent decline in mental processes including memory loss, impaired reasoning, and personality changes. Alzheimer’s disease is the most common form of dementia followed by vascular dementia, Lewy body dementia, and frontotemporal dementia. It is the 7th leading cause of death in the United States and does not have a cure.
Caring for a loved one with Alzheimer’s disease, vascular dementia, or any other form of dementia is challenging as the individual’s personality changes and cognitive function declines. They may even stop recognizing their nearest and dearest friends and relatives. As the disease progresses, they will require more and more care.
As a family caregiver, it’s important to be able to recognize the signs that death is near with dementia. When necessary, hospice can help by offering care wherever the individual resides, providing physical, emotional and spiritual care to the patient and support to their family.
10 signs death is near in dementia patients.
Understanding vascular dementia end-of-life symptoms as well as the final stages of death from Alzheimer’s or any other form of dementia helps ensure these patients receive appropriate care. These signs include:
- Increased physical weakness.
- Decreased appetite and thirst.
- More frequent and longer periods of sleep.
- Communication difficulties.
- Changes in behavior.
- Increased infections or susceptibility to infections.
- Incontinence.
- Difficulty swallowing.
- Labored breathing or changes in breathing patterns.
- Changes in skin color and temperature.
What is sundowners syndrome dementia connection – Search
Sundowner’s Syndrome at the end of life is also common, although it can also occur during earlier stages. Sometimes referred to as “sundowning,” this symptom describes the worsening confusion, anxiety, and agitation that patients experience late in the afternoon and evening.
Timeline for end-stage dementia in the elderly.
It can be difficult to know when dementia patients are near the end of their life because of the nature of the disease’s progression, but understanding what symptoms are most common at what times can help ensure the patient receives the right care. Below is a timeline of signs of dying in elderly people with dementia:
Final Six Months
- A diagnosis of another condition such as cancer, congestive heart failure or COPD
- An increase in hospital visits or admissions
Final Two-to-Three Months
- Speech limited to six words or less per day
- Difficulty in swallowing or choking on liquids or food
- Unable to walk or sit upright without assistance
- Incontinence
Final Days/Weeks
- Hands, feet, arms and legs may be increasingly cold to the touch
- Inability to swallow
- Terminal agitation or restlessness
- An increasing amount of time asleep or drifting into unconsciousness
- Changes in breathing, including shallow breaths or periods without breathing for several seconds or up to a minute
When are dementia patients eligible for hospice care?
Patients with dementia are eligible to receive hospice care if they have a diagnosis of six months or less to live if the disease progresses in a typical fashion. Once a patient begins experiencing any of the above symptoms, it is time to speak with a hospice professional about how they can help provide added care and support.
Benefits of Jigsaw Puzzles for Seniors: 15 Reasons Why I Regularly Do Jigsaw Puzzles – Gamesver
Tips for managing dementia end-of-life signs.
Because individuals with advanced dementia will often have difficulty communicating, it is important that caregivers keep a close eye on their loved one for signs of pain or discomfort. These signs may include moaning or yelling, restlessness or an inability to sleep, grimacing, or sweating. This may also signal that it’s time to call hospice or a palliative care team to help with the pain management.
If an individual with end-stage dementia is having trouble sitting up without assistance, hospice can provide a hospital bed or other equipment to lift their head.
Perhaps the hardest thing for families is when a loved one with dementia is no longer able to eat or swallow. Because an individual with dementia is unable to understand the benefits of feeding tubes or IV drips, they will often be incredibly distressed and attempt to remove them, causing added pain and risk of infection. Instead, focusing on keeping the individual comfortable. Supporting them with mouth care to prevent their mouth from becoming dry will allow them to make their final transition in peace.

What are the common dementia symptoms and tips to deal with dementia behaviors?
8 Common Dementia Behaviors and How to Manage Them
Here are some warning signs of dementia to watch for:
- Memory loss that disrupts daily life, such as forgetting recently learned information. 1
- Difficulty planning or solving problems, like trouble following a recipe or keeping track of monthly bills. 1
- Confusion with time or place, including losing track of dates, seasons, and the passage of time. 1
- Changes in mood and personality, such as becoming confused, suspicious, depressed, or anxious. 1
- Withdrawal from work or social activities, leading to a loss of interest in hobbies or social engagements. 1
If you notice these signs, it may be beneficial to consult a healthcare professional for further evaluation.
10 Early Signs and Symptoms of Alzheimer’s & Dementia | alz.org
11 Early Signs of Dementia: What to Watch Out For
15 Early Warning Signs and Symptoms of Dementia
What you can do for your loved one.
As an individual with dementia declines, you can help them by providing a loving and supportive presence. Sit with them. Hold their hand. Play music they enjoy.
One of the greatest gifts you can give your loved one is helping to get their affairs in order. Ensure that financial and healthcare powers of attorney are put in place, so you can make decisions when your loved one is no longer able. Look into funeral arrangements before you need them, so you don’t need to make important decisions in a time of crisis.
Talk to your loved one’s physician about the possibility of palliative care support in the home and hospice care when your loved one is ready.
How hospice can help with end-stage dementia.
In addition to helping you recognize the signs that death is near in patients with dementia, bringing in hospice care will help with the physical and emotional demands of caregiving. Nurses will be able to adjust medication and care plans as the individual’s needs change. Aides can help with bathing, grooming, and other personal care. Social workers can help organize resources for the patient and family. Chaplains and bereavement specials can help the family with any emotional or spiritual needs. Additionally, family members can contact hospice at any time, and do not need to wait until it is recommended by the patient’s physician.
To learn more about the criteria for hospice eligibility or to schedule a consultation, please call us at 855-905-2803 to speak with a hospice professional 24/7, choose one of the contact options in the bar above, or view our hospice service areas to find care in your area.
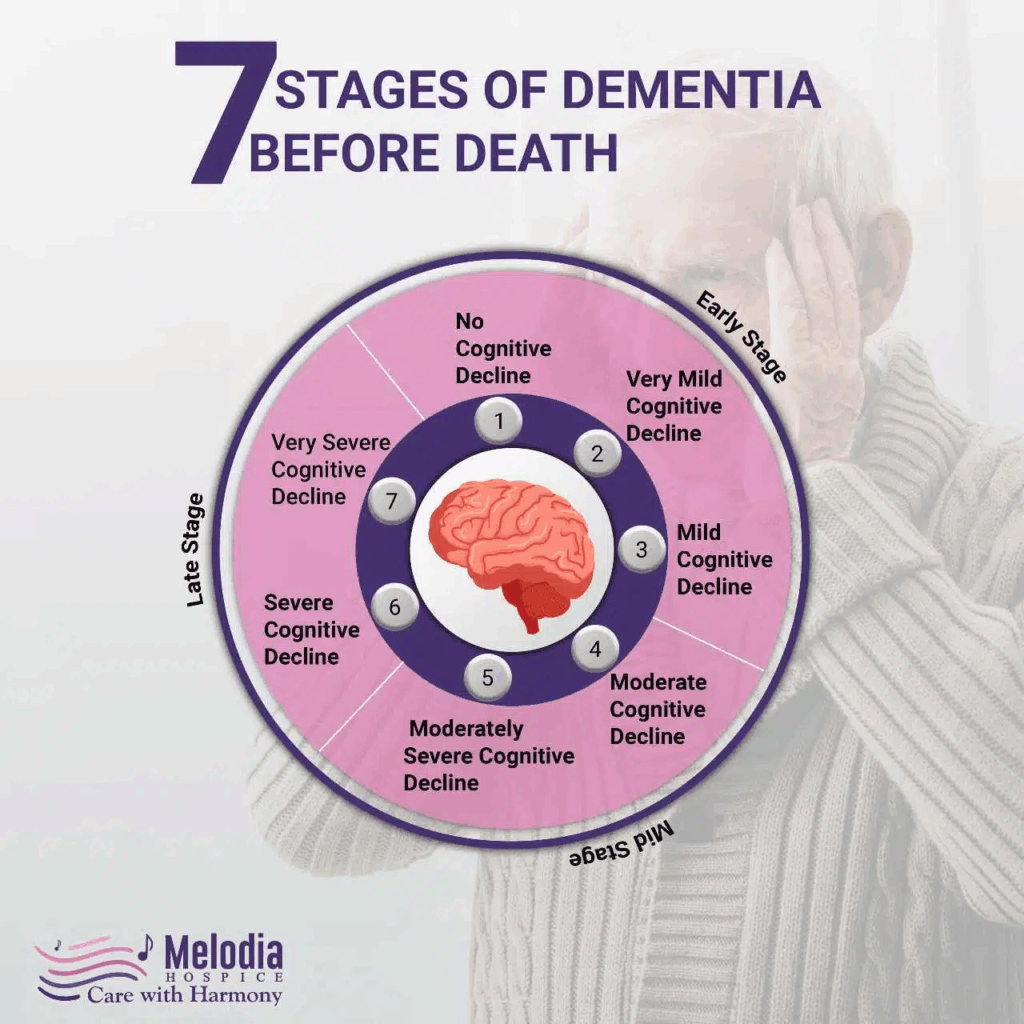
Infographic: 7 Stages of Dementia Before Death | Melodia Hospice
Overview
We all feel our moods change from time to time. People living with dementia, however, can experience an absence of interest in or concern about emotional, social, spiritual, philosophical or physical life.
They may become depressed or withdrawn and lose interest in activities they used to enjoy. Sometimes, they may lose the ability to manage their emotions.
It is important to remember that even in the later stages of dementia, the person is still able to experience a variety of emotions such as joy, love, fear and sadness. Provide support to ensure they are able to enjoy each day as fully as possible.
What is depression?
Depression is a condition in which people feel sad, hopeless or irritable most of the time. People with depression also experience anxiety and feelings of isolation. The number of people with depression rises over the age of 65.
Up to 40 to 50 percent of people with dementia experience depression at some point. Depression can make the symptoms of dementia worse. For example, depression can cause increased forgetfulness, confusion, and anxiety.
It is important to diagnose depression in people with dementia because depression may respond to treatment.
The symptoms of depression can be similar to symptoms of dementia. Therefore, it is often difficult to identify depression in people with dementia. There are some common signs of depression to be aware of:
- Loss of interest in previously enjoyed activities
- Lack of energy
- Problems sleeping
- Increased confusion
- Loss of appetite and weight
If you are concerned about depression, speak to the person’s doctor.
What is apathy?
Apathy is a word that describes loss of interest, motivation and/or persistence. It means not caring and not being social with others. The person with dementia may develop this apathy (become apathetic) and feel unmotivated to do anything. Apathy can be a symptom of depression but it can also occur separately from depression.
It can be distressing for a caregiver or family member to see the person with dementia withdrawing from social gatherings and other activities. Understanding the causes of apathy and how to respond to it can be helpful.
Possible causes of depression
- In the early stages of dementia, the person may experience depression after hearing their diagnosis.
- Social isolation may also cause depression in some people with dementia.
- Fatigue is associated with depressive symptoms.
- Depression can be a side effect of certain medications. Ask the person’s doctor to review the drugs they are currently taking.
Possible causes of apathy
- Apathy happens because the frontal lobe, an area of the brain responsible for planning, judgment, and insight, becomes damaged.
- Apathy may also happen to a person with dementia who does not understand what is happening.
If you are worried about any of these symptoms, talk to your family doctor.
Tips and strategies
Responding to depression
- Encourage pleasant activities that the person can still enjoy, such as short walks or outings.
- Set realistic expectations. If you expect too much from a person, they may feel frustrated and discouraged.
- Establish a consistent daily routine. This will help reassure the person as well as reduce confusion.
- Counselling, cognitive behavioural therapy, and group therapy may be helpful.
- Antidepressant medications may help. Talk to the person’s doctor about the options.
Responding to apathy
- Try to engage the person with dementia in activities that they enjoy.
- Make sure that they can participate at all levels and that they are not overwhelmed.
- Try introducing a small amount of the activity at a time.
- Choose flexible activities that can be changed to suit the person’s needs.
- Emphasize more on the process of doing things and not the results.
- Avoid activities where the person may not be able to complete the task.
- Make the person feel valued and productive.
- Be ready to help the person start an activity.
- Make the person with dementia feel included in groups.
- Have the person participate in activities that do not require active participation, such as listening to music.
- Some people with dementia may respond to a type of medication called a cholinesterase inhibitor. You may want to discuss this with a doctor.
More information and resources
Behaviours in Dementia Toolkit by the Canadian Coalition for Seniors’ Mental Health is an online library of over 200 free resources to help care partners and health-care providers better understand and compassionately respond to dementia-related changes in mood and behaviour.
Depression – Older Adults and Care Partners by the Canadian Coalition for Seniors’ Mental Health includes resources on depression and prevention of suicide in older adults.
Shifting focus: Guide to understanding dementia behaviour by the Alzheimer Society of Ontario and Behavioural Supports Ontario is meant to help family members, friends and caregivers of people with dementia understand behaviours and actions.
Distinguishing apathy from depression in neurocognitive disorders by Canadian Consortium on Neurodegeneration in Aging (CCNA). A tool for health-care providers to distinguish apathy from depression in neurocognitive disorders.
